Last Updated on March 11, 2024 by admin
You’ve taken an oath as a healthcare provider to provide the best possible care to your patients. However, as a practice owner, you must also take care of the financial side of your business. You or your staff must follow the ten steps in the medical billing process as part of your revenue cycle management.
This process begins when a patient comes to you, either in person or remotely (via telemedicine, for example), and ends when you receive payment. There will be communication between your office and health insurers, as well as between your office, your employees, and your patient.
It can sometimes appear complicated, especially if you’re starting in private practice. However, if you constantly follow the medical billing process, you will streamline the process, reduce errors, and receive payment for your services on time.
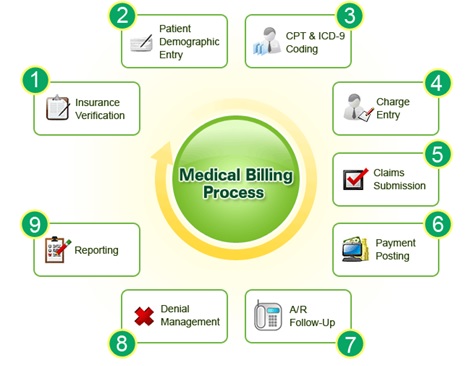
The Medical Billing Process in Ten Steps – How do medical billing companies in the USA do it?
These ten steps in the medical billing process will provide a solid foundation for the business side of your practice. Billing errors cost the healthcare industry billions annually (hospitals, private practices, insurance companies, and patients). This procedure will assist in reducing the number of mistakes.
- Registration of Patients
- Check Insurance
- Keep Track of Patient Data
- Send information to the billing team and use the appropriate codes.
- Charge Entry Review/Claim Filing
- Insurance Dispute Resolution
- Make a Patient Statement
- Patient Adherence
- Patient follow-up for payment
Registration of Patients
It doesn’t matter if this is your patient’s first visit or seeing you after years; it must include some form of patient registration. If it’s the 1st time, you need to record a complete medical history, including demographic details, which should be obtained for record-keeping purposes.
Regardless of whether the patient is a regular, double-check key details (home address, contact, and insurance) to ensure all info is updated and latest. Confirming an address or date of birth right away ensures that new information is added to the correct patient’s file.
Check Insurance and Financial Responsibility
Ensure that you have the latest and correct insurance coverage on the patient file during patient registration. This step allows you to ensure that you possess accurate insurance information, that the patient is generally covered, and that you have reviewed their out-of-pocket expenses. Confirming this data will assist in avoiding future delays and billing errors.
Take Notes of Patient Visits
Jot down all of the details shared during the initial consultation of the visit. If feasible, document the meeting (audio or video) or take thorough notes—all of this data will have to be given to a medical coder after the visit to apply the appropriate codes.
Following the visit, the meeting can be transcribed. Check that the reason for the visit is apparent, that any test results are included, that any prescriptions are listed, and so on. Not only will this benefit your coding/billing team, but it will also provide your patient with a more comprehensive medical history for future use.
Send Patient Data to the Billing Department
The medical transcription, also known as a medical script, of the visit is then cleaned up and prepared for the medical billing team. If you do this in-house, you can submit the recording to your staff, who can transcribe the notes. If you’re billing through a third party, ensure the medical script is error-free.
This is a critical step in the process where many errors can occur. You’ll make things easier for your coders, medical billers, and patients if you’re clear, concise, and thorough during the transcription.
You or your coding professionals will allocate the appropriate CPT or HCPCS code for your services. Choose the code that best describes the service performed, and ensure that any component services bundled with the primary procedure are not billed separately.
Following that, you or your coders must select the appropriate ICD-10 codes for the patient’s diagnosis. There are approximately 68,000 codes to choose from. The previous iteration (ICD-9) had about 13,000 codes to choose from—nearly five times as many codes to sort through! That is one of the factors contributing to the significance of the information you enter in the patient’s medical file.
Charge Entry
Your billing team will create a medical claim based on the codes assigned to the visit. That is why it is critical to use the correct codes—an incorrect code can drastically alter the charges. And, while the codes are uniform, the fees are not.
Ensure that all fees and the appropriate visit codes are listed. You can reduce errors and streamline the process by clearly itemizing medical services. Any mistakes could lead to claim denials, non-payment, or refund from the insurer, and claim denials. It can also impact how much your patient pays out of pocket.
Examine and File Claims
The claims are submitted for reimbursement after they have been reviewed for accuracy. This can be done electronically and usually involves a scrubbing phase followed by another review process. The software ensures that all form fields are completed and that the corresponding codes and fees are correct.
The claims are then routed to a clearing house for final review. Before reformatting the claim for particular payers—not all payers use a standard format—they undertake a final check of essential information (name, date of birth, and active insurance checks).
Patient Follow-up and Payment
The final step is receiving payment from the insurer and the patient. When insurance companies accept claims, payments are frequently made automatically. Patients can pay for a visit in advance (co-pay) or before the procedure. Other people often choose to pay at various times.
Although each step is critical, paying for your services enables you to earn a profit, pay your employees, and keep the lights on. You must give your patients a certain amount of time to begin producing, but you could be forced to go through collections.
To find out more about “medical billing in the USA” and why Medphine is considered one of the “best medical billing companies,” get in touch with our specialists.